Shoulder pain is an extremely common complaint, and there are many common causes of this problem. It is important to make an accurate diagnosis of the cause of your symptoms so that appropriate treatment can be directed at the cause. If you have shoulder pain, some common causes include:
Bursitis | Rotator Cuff Tendonitis
The most common diagnosis in patients with shoulder pain is bursitis or tendonitis of the rotator cuff.
Rotator Cuff Tear
Rotator cuff tears occur when the tendons of the rotator cuff separate from the bone. Surgery is sometimes necessary for this condition.
Frozen Shoulder
Also called ‘adhesive capsuliitis,’ this is a common condition that leads to stiffness of the joint. Physical therapy and stretching are extremely important aspects of treatment.
Calcific Tendonitis
Calcific tendonitis is a condition of calcium deposits within a tendon — most commonly within the rotator cuff tendons. Treatment of calcific tendonitis depends on the extent of symptoms.
Shoulder Instability
Instability is a problem that causes a loose joint. Instability can be caused by a traumatic injury (dislocation), or may be a developed condition.
Shoulder Dislocation
A dislocation is an injury that occurs when the top of the arm bone becomes disconnected from the scapula.
Shoulder Separation
Also called an AC separation, these injuries are the result of a disruption of the acromioclavicular joint. This is a very different injury from a dislocation!
Labral Tear
There are several patterns of a torn labrum and the type of treatment depends on the specific injury.
SLAP Lesion
The SLAP lesion is also a type of labral tear. The most common cause is a fall onto an outstretched hand.
shoulder impingement
Shoulder impingement is a condition characterized by pinching or compression of soft tissue, such as the rotator cuff tendons and the subacromial bursa, between the upper arm bone (humerus) and roof of the shoulder (acromion) during certain movements of the shoulder, such as arm elevation.
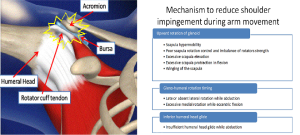
The shoulder joint is a ball and socket joint. The socket arises from the outer aspect of the shoulder blade, whilst the ball arises from the upper aspect of the humerus (upper arm bone). Just above the ball and socket joint of the shoulder is a bony prominence known as the acromion (figure 1). Beneath the acromion lie the tendons of the rotator cuff muscles and the subacromial bursa (figures 1 & 2). The rotator cuff muscles are a group of four muscles (supraspinatus, infraspinatus, subscapularis and teres minor) which primarily act to stabilize the shoulder joint and assist with shoulder movements (figure 2). A bursa is a small sac filled with lubricating fluid, designed to reduce friction between adjacent soft tissue or bony layers. The subacromial bursa reduces friction between the bony prominence of the acromion (above the bursa) and the rotator cuff tendons (in particular the supraspinatus tendon, which attaches to the upper aspect of the humeral head – below the bursa).
Occasionally due to injury associated with overuse or a specific incident, the rotator cuff tendons or subacromial bursa may become damaged, swollen and inflamed. As a result of the swelling, the rotator cuff tendons or subacromial bursa may occupy more space and can subsequently become compressed or pinched during certain movements of the arm, such as elevation (as the humeral head below moves towards the acromion above). Several other postural, biomechanical or anatomical anomalies (such as bony spurs or arthritis) may also contribute to this process. When this occurs the condition is known as shoulder impingement. Shoulder impingement can also sometimes involve the long head of biceps tendon.
Causes of shoulder impingement
Since the rotator cuff tendons and subacromial bursa lie in a very small space between the acromion and humerus, anything that narrows this space may cause shoulder impingement. Shoulder impingement most commonly occurs in association with rotator cuff tendonitis or subacromial bursitis (i.e. inflammation of the tendon(s) or bursa respectively). These conditions typically occur due to repetitive or prolonged activities placing strain on the rotator cuff tendons and/or subacromial bursa. This may occur during repetitive arm elevation activities, overhead activities, reaching activities far away from the body, activities involving rotation of the shoulder, lifting (especially overhead), pushing or pulling activities, placing weight through the affected arm or lying on the affected side. Occasionally, these conditions may occur suddenly due a direct blow to the point of the shoulder, a heavy or awkward lift or due to a fall onto the shoulder, elbow or outstretched hand. Patients with muscle imbalances, shoulder instability, poor posture, or poor shoulder blade control may also have an increased likelihood of developing shoulder impingement.
In athletes, shoulder impingement is commonly seen in throwing sports (such as cricket or baseball), swimming (particularly freestyle and butterfly), racquet sports (such as tennis), weight lifting or paddling sports (such as kayaking). Anomalies to the acromion bone, degenerative changes to the AC joint, or bony spurs known as osteophytes, may also predispose a patient to developing shoulder impingement.
Signs and symptoms of shoulder impingement
Patients with shoulder impingement typically experience pain at the top, front, back or outer aspect of the shoulder. Pain may also radiate into the upper arm as far as the elbow, usually along the outer aspect or down the biceps muscle. Symptoms typically increase during activities that compress the rotator cuff tendons or subacromial bursa. These activities may include arm elevation activities, overhead activities, reaching activities, shoulder rotating activities, lifting, throwing, pushing or pulling, placing weight through the arm or lying on the affected side. In patients with minor shoulder impingement, little or no symptoms may be present. Some patients may experience pain on commencing activity that reduces as they warm up. These patients are usually able to continue sport or activity only to have an increase in pain, ache or stiffness upon resting later (particularly that night or the following morning).
As the condition progresses, patients may experience restricted shoulder range of movement and symptoms that increase during activity or sport, affecting performance. Patients with shoulder impingement may also experience pain on firmly touching the top / outer aspect of the shoulder. A painful arc of arm elevation and / or a feeling of shoulder weakness may also be present particularly when attempting to lift, throw or elevate the arm overhead.
Diagnosis of shoulder impingement
A thorough subjective and objective examination from a physiotherapist is usually sufficient to diagnose shoulder impingement. An ultrasound investigation is commonly used to identify associated conditions, such as rotator cuff tendonitis or subacromial bursitis, and may also demonstrate shoulder impingement on assessment during arm elevation. Further investigations such as an X-ray, CT or MRI scan are often used to assist diagnosis and determine the presence of other conditions.
Prognosis of shoulder impingement
Most patients with this condition heal well with appropriate physiotherapy and return to normal function in a number of weeks. Occasionally, rehabilitation can take significantly longer and may take many months in those who have had their condition for a long period of time, or, in those with other associated significant injuries such as shoulder instability, rotator cuff pathology or degenerative bony changes, such as arthritis. Early physiotherapy treatment is vital to hasten recovery in all patients with shoulder impingement.
Treatment for shoulder impingement
Most cases of shoulder impingement settle well with appropriate physiotherapy. The success rate of treatment for this condition is largely dictated by patient compliance. One of the key components of treatment is that the patient rests from any activity that increases their pain until they are symptom free. Activities which place large amounts of compressive forces through the rotator cuff and subacromial bursa should be minimized, these may include: arm elevation or overhead activities, reaching away from the body, throwing, heavy lifting, pushing or pulling and sleeping or lying on the affected side. Resting from aggravating activities ensures that the body can begin the healing process in the absence of further tissue damage. Once the patient can perform these activities pain free, a gradual return to these activities is indicated provided there is no increase in symptoms.
Ignoring symptoms or adopting a ‘no pain, no gain’ attitude is likely to cause further damage and lead to the condition becoming chronic. Immediate, appropriate treatment in patients with shoulder impingement is essential to ensure a speedy recovery. Once the condition is chronic, healing slows significantly resulting in markedly increased recovery times and an increased likelihood of future recurrence.
Patients with shoulder impingement should follow the R.I.C.E regime in the initial phase of injury. The R.I.C.E regime is beneficial in the first 72 hours following injury onset or when inflammatory signs are present (i.e. morning pain or pain with rest). The R.I.C.E. regime for shoulder impingement primarily involves resting from aggravating activities and regular icing. Anti-inflammatory medication may also significantly hasten the healing process by reducing the pain and swelling associated with inflammation.
Manual “hands-on” therapy from the physiotherapist such as massage, trigger point releases, joint mobilisation, manipulation, dry needling, stretches and electrotherapy can also assist with hastening healing and improving flexibility and function in patients with this condition.
Patients should also undergo a graduated flexibility and strengthening program of the surrounding muscles to ensure an optimal outcome. Particular emphasis is placed on improving shoulder blade stability, posture and rotator cuff function. The treating physiotherapist can advise which exercises are most appropriate for the patient and when they should be commenced.
Often, a corticosteroid injection by a sports physician into the subacromial bursa or affected rotator cuff tendon is effective in reducing symptoms and allowing earlier rehabilitation progression.
In the final stages of rehabilitation, a gradual return to activity or sport can occur as guided by the treating physiotherapist provided there is no increase in symptoms.
In patients with significant pathology involving major rotator cuff pathology and/or bony spurring, orthopaedic surgery may be considered to improve the condition.
Contributing factors to the development of shoulder impingement
There are several factors which can predispose patients to developing shoulder impingement. These need to be assessed and corrected with direction from a physiotherapist. Some of these factors include:
- joint stiffness (particularly the shoulder, neck or upper back)
- shoulder instability
- bony anomalies of the acromion or AC joint
- muscle tightness (particularly the rotator cuff, pectorals and deltoid)
- poor posture
- inappropriate or excessive training
- inadequate warm up
- muscle weakness (especially the rotator cuff and scapula stabilisers)
- muscle imbalances
- inadequate rehabilitation following a previous shoulder injury or surgery
- inappropriate technique (e.g. swimming stroke, tennis serve, throwing technique)
Physiotherapy for shoulder impingement
Physiotherapy treatment is vital to hasten the healing process, ensure an optimal outcome and reduce the likelihood of recurrence in all patients with shoulder impingement.
- soft tissue massage
- electrotherapy (e.g. ultrasound, TENS etc)
- stretches
- joint mobilization
- joint manipulation
- ice or heat treatment
- exercises to improve strength, flexibility, posture and scapula stability
- correction of abnormal biomechanics or technique
- education
- postural taping
- the use of a postural support
- anti-inflammatory advice
- activity modification advice
- a gradual return to activity program

![shoulder[1]](https://www.sakariyaphysio.com/wp-content/uploads/2013/04/shoulder1-300x203.jpg)